Stats don’t support Public Health assertion that travel is largely responsible
UPDATED: Statistics current as of Tuesday, May 26
According to statistics released by Niagara Region Public Health on Tuesday, May 26, the municipality of Pelham has seen the second-highest rate of historic COVID-19 infections on the Niagara peninsula since the start of the pandemic.
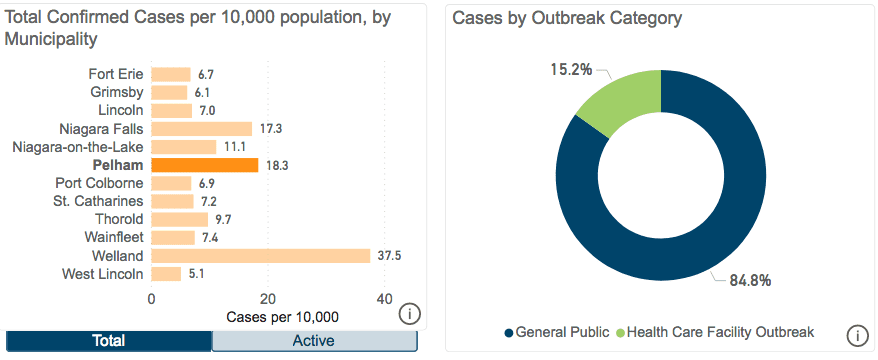
Pelham’s rate is 18.3 infections per 10,000 residents, far exceeding lower rates seen in eight other Niagara towns.
Welland is highest, with 37.5 infections per 10,000 residents.
West Lincoln’s rate is the lowest, at 5.1. Seven communities have an infection rate of below 8 per 10,000 residents.
Only Niagara Falls approaches Pelham, with 17.3 infections per 10,000 residents. However, in Niagara Falls, some 60 percent of cases are tied to healthcare facilities.
There is currently one active infection in Pelham, and the town’s current infection rate is tied for the second lowest in the Region.
“Part of the reason why Pelham has a higher cumulative proportion of cases is that it had proportionally more international travel-related cases in the early weeks of local COVID-19 transmission,” Public Health spokesperson Kerri Stoakely told the Voice.
“Beyond that it is likely due to statistical variation as we have not seen any large clusters of linked infections.”
Yet the Health Department’s own numbers don’t support Stoakley’s assertion.
In fact, the number of travel-related cases in Pelham is less than half of the non-travel-related cases.
Niagara-on-the-Lake, with similar demographics to Pelham, has by far a proportionately greater number of travel-related cases than does Pelham. And Fort Erie turns the tables entirely, with more than double the number of travel-related versus non-travel-related infections.
COVID-19 cases by outbreak category are also notably different in Pelham.
In other Niagara towns, a relatively larger percentage of outbreaks are categorized by Public Health as having occurred in healthcare facilities.
In Pelham, however, 85 percent of infections have occurred among the general public, with just 15% occurring in healthcare facilities, which include long term care and retirement homes.
The only other community with a higher infection rate among the general public is again the demographically similar Niagara-on-the-Lake, where just 1 in 10 infections were tied to healthcare facilities, while 9 in 10 were among the general public.
As of the 2016 census, 17,100 residents called Pelham home. Public Health says that there have been some 33 confirmed cases of COVID-19 in the municipality since the start of the pandemic.
Four individuals who later tested positive for the virus shared the same enclosed space, during Pelham Town Council’s meeting of March 23. Councillor Ron Kore, Councillor Mike Ciolfi, and two senior administrators all later tested positive for COVID-19. The two staffers and Kore experienced varying symptoms and recovered. Councillor Ciolfi died ten days later. An official cause of death has not been made public.
On April 22, news broke that Kore, who is also the Fonthill Sobeys franchisee, had continued working in his store and attending council while exhibiting symptoms of a respiratory illness. A Sobeys corporate spokesperson said at the time that under public health guidelines the store employees didn’t need to be tested.

That week and into the weekend, Mayor Marvin Junkin and Pelham Regional Councillor Diana Huson made repeated requests of Niagara Public Health to offer testing to all Fonthill Sobeys employees regardless of whether they were symptomatic. A conference call on Sunday, April 26, between them, Regional Chair Jim Bradley, Acting Medical Officer of Health Dr. Mustafa Hirji, and others, ended the way it started. There would be no exception made to the testing criteria then in place.
Junkin told the Voice that if he knew then what Public Health has released now, he would have lobbied harder for testing.
“I am very disappointed that I have not been kept in the loop by Niagara Regional Health. Not once have I been contacted by this organization to inform me of this startling statistic. Ms. Huson and I pressed for testing of local Sobeys workers to no avail. If we had known before [the April 26 conference call] that Peham had that many more cases than our neighbours, Diana and I would have pressed harder for more testing.”
Huson said that in her view the data did not point to any clear conclusion.
“It could suggest a number of things,” said Huson. “Our numbers could skew higher due to our proximity to Welland, who have seen the largest number of cases. Alternatively it could be because our population skews towards an older demographic, who have been affected at much higher rates.”
Like Junkin and Huson, Pelham CAO David Cribbs had not been informed of the data by Public Health before being contacted for comment by the Voice.
“The Town did not have previous access to this data and the data can only be described as an unpleasant surprise,” said Cribbs. He echoed Huson’s concerns about drawing conclusions.
“The Town has no context for the data—did these cases occur at the start of the pandemic, are they very recent, or has there been a consistent rate of infection? Has there an outbreak that was not identified or reported? Are the Town’s demographics of being older than the Provincial and Niagara average a contributing factor? The raw data provided simply does not tell the full story.”
“It should be remembered that numbers in many municipalities, including Pelham, are small,” said Public Health spokesperson Kerri Stoakley, “and so large variations can be apparent with only a few cases.”
Dr. Mustafa Hirji, Acting Medical Officer of Health for the Niagara Region, told the Niagara-on-the-Lake Local that the numbers don’t identify where the virus was contracted, but where those with the virus live.
“They could been having coffee in St. Catharines, gone to work in Thorold and then done some grocery shopping in Niagara Falls on the way home,” Hirji said, and have no idea where they contracted it.
“There are limitations of what we can interpret from the data. This represents the cases we know about, and not where they were exposed to it.”
The main takeaway from the statistics, Hirji said, “is that people in every municipality have been infected, and it’s still out there. We still have a small number of cases every day. As businesses are opening up, and we have the potential for interacting, we have the potential for the virus to spread."
From the beginning of the outbreak, despite pressure from elected officials across the region, Hirji had refused to release COVID-19 statistics per municipality, citing privacy concerns. The small numbers in most municipalities might have made it possible to identify individuals, he said.
About two weeks ago, Hirji told the NOTL Local that cases might be getting to the threshold where he would be willing to release that information. Niagara crossed that threshold last Wednesday, the day Wainfleet reached five cases.
He is not breaking down the numbers of deaths per municipality. Hirji said he may in coming weeks consider releasing more numbers related to deaths, such as those in retirement homes, long-term care homes, hospitals, and even by age group, “in the interest of transparency,” but he doesn’t expect to release numbers per municipality.
Although the numbers represent positive tests, not the overall infection rate among those who may be positive but asymptomatic, Hirji said he was confident they are a realistic indication of “the big picture.”
If people started showing up at the hospitals and require intensive care, there might be concern that the numbers are not accurate, “but we’re not seeing that.”
Hirji stressed that the best advice now is for people who are experiencing COVID-19 symptoms to reach out to assessment centres or their physicians for advice about whether to be tested. With sufficient capacity for testing now available, he said, anyone who has symptoms can be tested.
“We really do want to find any cases that are out there.”
David Cribbs and Diana Huson both pointed to the statistics as a reminder that the pandemic hasn’t gone anywhere.
“Certainly this reinforces the need to continue practicing all of the personal hygiene and social distancing guidelines recommended by health authorities,” said Cribbs.
“All we really know,” said Huson, “is that it is vitally important to continue with thorough hand washing practices, physically distancing from one another, and staying home when possible to help prevent a second wave from further crippling our communities.”
Find Niagara Public Health COVID-19 updates here.
With reporting by Dave Burket and John Chick, and files from the NOTL Local.
UPDATED May 26, 9:15 PM, with current Public Health statistics
UPDATED May 23, 5:45 PM, with comment from Dr. Mustafa Hirji


