Once we reach 18 years old, and can do all those things that become much less exciting once they’re legal, few of us strive to purposely look older than we are. By 30 we’re wary of any visual hint that we’re aging, at 50 our body image battle begins in earnest.
Few things imply old more clearly than kyphosis, or excessive curvature of the spine; that 18th century look our ancestors had when struggling under the weight of a sack of grain.
Back and spinal problems caused by Scheuermann’s disease, multiple sclerosis, spinal bifida, and other conditions can be debilitating and extremely painful. This column addresses the varieties of kyphosis which can be corrected, cured or postponed with lifestyle changes, even if you’re not lucky enough to have a partner like mine who constantly reminds me to, “stand up straight.”
Unfortunately, kyphosis doesn’t just affect older adults. It is in part a disease of our time. Many younger people engage in activities that increase the risk of slouching. As we spend more time hunched over our computer screens and phones, posture and proper body alignment deteriorate, increasing the stress on our spine, discs and muscles.
The recent dramatic increase in depression and anxiety across all age groups is an additional factor. These emotions can trigger lethargy, often displayed with a slouching head down posture, a precursor to kyphosis.
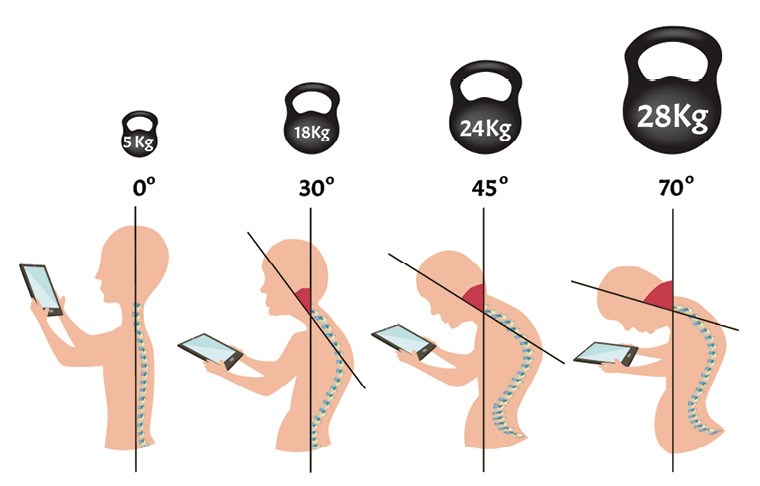
What is kyphosis and how is it caused? Our spine is subdivided into three specific areas. Cervical spine refers to the neck area, thoracic spine is the middle portion, extending down to the vicinity of our diaphragm, and the lumbar spine is our lower back. Normal posture manifests itself as a straight or very gently ‘S’ shaped spine, with the lower back protruding forward very slightly and the upper back (thoracic spine) curved forward to a maximum of 35 degrees. Kyphosis occurs when the curvature of the upper spine exceeds 40 to 45 degrees.
Our vertebral column is composed of bones (vertebrae), gelatin-like cartilage called intervertebral discs, and muscles. Age and disease affect all three components, often resulting in stooped posture.
As we age our ability to process calcium decreases. Beginning after age 65 in men and post-menopause in women, our bones become less strong and dense and increasingly brittle. Osteoenia is a milder form of osteoporosis which also causes our bones to lose calcium and shrink.
Our discs lose flexibility and harden as we age, which causes them to compress. Our weight and normal spine curvature cause us to lean forward, which means our discs compress into a wedge shape. The result of this wedge-shaped compression is even more forward tilt, eventually leading to kyphosis.
Our back or spine is supported by three main muscle groups. Extensor muscles, including the large erector spinae group located in the lower back, are attached to the back of our spines, allowing us to lift and stand. Flexor muscles, including our abdominals, are attached to the front of the spine and allow us to bend forward as well as arch our backs. Oblique muscles attached to the sides of our spine allow us to rotate our bodies. These three muscle groups are responsible for our posture. Loss of strength in these muscles as we age also contributes to kyphosis, as does the normal redistribution of body fat to our waists.
Kyphosis can not only rob us of our appearance of youth, it can also accelerate physical aging by increasing the chance of other health issues. As your spine curves forward, your rib cage presses on your lungs and diaphragm, making deep-breathing more difficult. It’s the flush of oxygen entering our blood stream and cells that allows quick energy recovery and a healthy cardiovascular system, one of the most important components to maintaining physiological youthfulness.
This internal organ compression may also create digestive issues such as acid reflux and difficulty in swallowing.
There are ways in which, at any age, we can combat kyphosis without medication. Understanding that spinal deterioration happens gradually over many years, we must also expect that a return to spinal health achieved by reversing naturally controllable factors may take months or up to a year. There is no quick fix, but the effort is worth it.
Healthy lifestyle choices are important to correcting posture issues. It may also be wise to consult a doctor or physiotherapist because various types and severity of kyphosis require different corrective strategies.
Note that plant protein is different than animal-based protein, which is high in saturated fat
Regular exercise and targeted weight-bearing activities are necessary to counteract the anticipated muscle and bone loss of aging. Abdominal flexor muscles need strength and flexibility to work cohesively with our large erector spinea muscles to provide good posture while standing erect. Range of motion and body alignment, good posture in general, will all improve with muscle balance.
Exercise also increases blood flow in the arteries that feed the spine, helping it remain supple and healthy. Various exercises including posture stretches, chin tucks, floor Y-stretches and prone extensions all increase the strength and suppleness of our muscles. Abdominal stretches on a Swiss ball and yoga positions such as the cobra and plank counteract our tendency to slouch.
Be conscious of personal risk factors in your daily ergonomics, and ensure good spine support. If you purchase “ergonomic” chairs, desks and other equipment, make sure they fit and you understand how to use them. Keep your feet flat on the floor, use a lumbar support, and don’t cross your legs. Tilt your chair to 100 – 110 degrees, don’t sit at 90 degrees. Keep screens at eye level to avoid craning your neck, and position your keyboard so your hands are lower than your elbows.
Stand or move around regularly. Our back and core muscles become weak and atrophied from lack of movement. Standing and walking lessens this muscle stiffness and fights misalignment of the spine, as well as promoting blood flow and removal of physiologic toxins which tend to accumulate in lower back muscle tissue.
Bend from the hips not your waist. Bending from the waist puts the whole weight of your torso and head on just one or two vertebrate and discs, while hip bending engages the strength of your spinal erectors and glute muscles for support.
Diet matters. A spinal health study published by the U.S. National Library of Medicine found that, “By age 49, 97 percent of the discs of those eating the Standard American Diet show at least grade-2 degradation,” a startling figure.
Choose calcium-rich foods that promote bone strength to reduce minute compression fractures. Consume sufficient muscle-building high-quality protein. Note that plant protein is different than animal-based protein, which is high in saturated fat. Animal-based protein causes inflammation which can exacerbate back pain and degeneration.
Look for foods high in Vitamin D, K, and magnesium.
Excessive alcohol use can upset the calcium balance in your body and inhibit absorption of vitamins and hormones necessary for strong bones. Smokers are more likely to have osteoporosis and bone fractures, and heal less quickly afterward than non-smokers.
Any steps we can take to postpone kyphosis are worthwhile for maintaining good body self-image, and most will furnish additional health benefits, especially as we age. ◆